Great Show Kathy Bates! We are so proud of your efforts toward Lymphedema Awareness and Research. →
Top 7 Reasons to get to the Lymphedema Awareness Walk March 28th 2015:
Movement and You:
1) Support Patients with Lymphedema and Breast Cancer Related Lymphedema.
All proceeds go toward assisting these patients with their care and supplies.
2) Cancer Prevention:
- Inactivity is strongly correlated to Cancer Risk.
- Movement prevents cancers.
- Common Side effects of cancer treatment are alleviated with exercise.
In the 2008 Journal of Clinical Oncology, women walking briskly 2-3 hours per week in the year prior to developing breast cancer were 31% less likely to die from the cancer than the sedentary women. Also, those women who increased their activity after diagnosis lowered their risk of death by 45%. Conversely, those decreasing their activity upon diagnosis increased their risk of death four-fold.
3) Enhances Strength and Density of Bones.
- Increases and maintains bone mineral density in older adults.
4) Prevents Diabetes:
- Maintains Normal Blood Sugar
- Improved insulin signaling
5) Improves Heart Health:
- Lowers Blood Pressure
- Lower Resting Heart Rate
- Improves Circulation
- Decrease Body Mass Index
6) Enhances Immunity:
- The strength of your immune system is directly correlated to physical activity.
- Can help prevent respiratory tract viral infections and reduce their duration.
7) Improved Mental Health:
- Improves image of Self
- Improves confidence
- Lowers Stress
- Improves Sleep
Source:
“Lise Alschuler, ND, FABNO, and Karolyn A. Gazella”
Peapod Purse
A Lymphedema Charitable Organization
5K Walk in Support of Lymphedema Awareness and Treatment
WHEN? Saturday March 28th, 2015 8am Registration/ 9am Start Time
WHAT? A 5K walk at the Manalapan Recreation Center
WHERE? Located at 120 County Road 522 in Manalapan, NJ
WHY? To support Lymphedema Awareness & Treatment
WHO? You!
For More Information or To Sign up Visit:
Peapod Purse 5K Walk for Lymphedema Patients
First Annual Lymphedema Walk for Charity Sponsored by The Peapod Purse Charitable Foundation.
For Online Registration and Donations go to the home of the Peapod Purse Lymphedema Charity (Clik) Or for Paper Registration (Clik)
Breast Cancer Related Lymphedema BCRL Undiagnosed in 36% of Patients with Lymphedema. 87% of Lymphedema Diagnosed Patients not receiving the Gold Standard of Care.
In a Nov. 2013 study of 450 Breast Cancer Survivors who had symptoms of Lymphedema after Breast Cancer Treatment, 36% had not been diagnosed with Lymphedema by their physician. Of the 64% of Breast Cancer Survivors who were diagnosed with Lymphedema, only 13% received the Gold Standard in Treatment consisting of Complete Decongestive Therapy CDT and Manual Lymph Drainage MLD with Compression Garments, and Remedial Exercises as defined by The National Lymphedema Network in their 2011 Position Statement.
This study at The Medical College of Wisconsin showed that despite very effective interventions for Breast Cancer Related Lymphedema, 87% of those diagnosed did not receive the Gold Standard of Care. It also demonstrated that 160 of 450 Breast Cancer Survivors were not diagnosed with Lymphedema despite symptoms.
Please see our section on Breast Cancer Rehabilitation for current research on Breast Cancer Related Lymphedema, early intervention, prevention, and lymphedema treatment. In the Jan. 2013 edition of Breast, BCRL or Breast Cancer Related Lymphedema was found to be the most common disease/ morbidity associated with Breast Cancer Treatment. Early Intervention with monitoring through measurement and bioimpedance is the most highly recommended way to minimize the occurrence of swelling and to get limb swelling under control fast.
Wyatt Rehab is a World Leader in Lymphedema Treatment and Wyatt uses The Gold Standard Treatment for Lymphedema. Wyatt is thoroughly versed in all procedures and devices and has helped thousand of patients since 2005. Contact Wyatt today if you are receiving Breast Cancer Treatment and have concerns about Lymphedema. Print this referral for your Physician and talk with them today.
Lifting Weights May Reduce Breast Cancer Lymphedema
Survivors of Breast Cancer who lift weights 2x per week with a slow progression have a lower incidence of Arm Lymphedema. After breast cancer treatment, incidence of "Breast Lymphedema", "Breast Cancer Lymphedema", "Breast Cancer Related Lymphedema" or "BCRL" often occurring in the arm, is decreased when working out. This is contrary to what some believe but was confirmed by U. Penn Center for Clinical Epidemiology published in a 2010 randomized trial in JAMA. Weight Lifting was introduced and Breast Cancer Survivors were monitored for a year including 13 weeks of supervised medical exercise instruction and 9 months unsupervised--134 participants took part.
Breast Cancer Lymphedema was decreased by 6% in those who performed exercise at least 2x per week. Breast Cancer Lymphedema occurred in only 11% of those that performed weight lifting while the control group had a 17% incidence of Lymphedema. Among the aforementioned, at least 2 nodes were removed. When the 49 participants who had 5 or more nodes removed were analyzed, their decrease was even greater dropping 15% compared to the control group.
Breast Cancer Survivors are encouraged to slowly work through a progression in weight training. This has been shown to reduce Lymphedema risks. Wyatt Rehab offers a Breast Cancer Rehabilitation Program that addresses these needs in a Physical Therapist supervised environment. Physical Therapists at Wyatt are experts in Breast Cancer Rehab, Breast Cancer Lymphedema, Physical Therapy, Lymphedema Prevention, and Lymphedema Early Intervention.
This research coupled with the 2012 study in Lymphology extolling tremendous benefits of Manual Lymph Drainage MLD for Breast Cancer Survivors provides extremely strong evidence for Breast Cancer Rehab Programs like those at Wyatt Rehab. The Lymphology study effectively suggesting MLD after surgery is preventative for Lymphedema- lowering the risk to near zero. Early intervention, monitoring programs, and preventative measures, e.g., MLD, Physical Therapy, and Medical Exercise Programs greatly reduce the incidence of Breast Cancer Lymphedema.
Exercise and Yoga for Breast Cancer Survivors
A 2013 retrospective meta-analysis in the Journal of Physiotherapy reviewed 34 studies to determine effectiveness of exercise programs in patients who had undergone treatment for Cancer. The results suggest tatistically significant benefits in body weight, peak oxygen consumption, strength, physical function, and quality of life for those patients involved in exercise after treatment. 65% of the individuals reviewed possessed Breast Cancer.
In 2013 The Department of Clinical Psychology at VU University Amsterdam performed focus groups to determine the effects of Yoga on Cancer patients. 29 Cancer Patients participated and 72 % were Breast Cancer Patients. Their mean age was 53. The results suggested physical and psychosocial benefits including: mental strength and resilience, increased physical fitness and function, relaxation, and happiness. These results exactly match a much larger 2012 study of 742 participants in BMC Cancer. These results support Breast Cancer Rehabilitation programs and Yoga for Breast Cancer survivors.
Furthermore, The International Journal of Yoga in January 2013 showed results from the Division of Yoga Life Sciences at SVYASA, a Yoga University in India. Approximately 30 individuals were tested for DNA damage through an electrophoresis assay. There were three groups tested: Yoga Practitioners, Breast Cancer Patients, and a Control Group of Non-Yoga Practitioners. 500 cells were assessed for DNA damage. The results showed significantly lower DNA damage in yoga practitioners.
My Day in a Compression Garment...
To honor the lymphedema patients that undergo intensive Complete Decongestive Therapy (CDT), some of our staff volunteered to be wrapped in layers of short stretch bandages on top of custom designed foam for National Lymphedema Awareness Day, March 6, 2013. Multilayered bandaging is just one of the components of CDT. The multiple layers of bandaging applied meticulously with constant tension and patterns of spirals and herringbones, create a compression gradient that is effective in improving lymph drainage from the limb. When applied, it looks and feels like a soft cast.
decided to challenge myself by working all day with a thigh high leg bandage. This unique opportunity gave me a better understanding of what my patients go through during the very treatment that I provide every day. Each one of my toes was wrapped individually and soft foams were customized to contour around my leg. Short stretch bandages were applied over the foams with unique patterns and spacing to achieve the appropriate compression gradient. Then it was off to work!
hroughout the day, I came across some challenges for sure. The first was walking in the firm rigid bandage that restricted my knee and ankle range of motion. I immediately began to compensate for the lack of knee flexion by hiking my hip. This didn't allow me to move as quickly as I usually do! Being that I chose to wrap my leg, I was able to provide Manual Lymph Drainage without any issues but bandaging my patients became challenging as I use my legs to stoop and squat down. I sometimes sit on the floor to wrap legs - I again had to move slowly with more caution and care knowing I couldn't bend my knee and sit on my heels. Whew, I treated one patient and it was off to the bathroom. Whoops, how do I do that? I have never had to concentrate so much during such a routine task of daily life. As I figured it all out, I was so excited that I didn't pee on my bandage in the restroom that I got up off the toilet and hit my head on the wall in front of me. While doing some documentation, I was sitting on my Theraball Chair and my leg began to fall asleep. Trying to get up and not fall over on my mildly bulky leg (and now tingly) was tricky but my leg woke up and I was off to an afternoon of patients. I made every attempt to continue going about my day as usual. I got through the afternoon with more grace as I was getting used to this new restriction. Then I had to drive home. Rushing out the door with all of my many bags lugged over my shoulders; I got to the front door and realized it was raining! I ran back in the clinic to get a rainproof bootie. Walking across the parking lot with this bootie, I pushed off with my little wrapped toes, feeling the chill of the pavement through the bootie. Pulling my left leg into the car, I took some time to position myself for the ride home. Ten minutes into my drive, my leg began to go numb again. I realized I had to correct the position of my driver seat so that the angle of my hip was toward the floor, allowing less compression on the sciatic nerve. I arrived home to be greeted by my husband and my 4 year old son. I was exhausted and ready to call it a day. The best part of my experience was watching the excitement in my son's eyes when I explained to him what I did all day. He had many many questions surrounding my experience. He wanted to know why my leg was wrapped like that, why was I walking funny, why I had so many bandages, why do my patients have to wear these bandages, why do I use cotton underneath, and "Mommy, why are your toes wrapped?" As he vigorously assisted me with unwrapping my leg, his excitement grew like my leg was a birthday gift all wrapped up in ribbons. At the very end, when the bandages were finally removed, we had a pile of unraveled bandages and foams and I thought "Ahhh, yes, this is where I have to get back up and do the laundry for the next day".
I am very thankful to have had this opportunity to celebrate our patients and to further my understanding of the great task of enduring a Multilayered Bandage. I just had a short glimpse of what my patients go through while being wrapped for Lymphedema Treatment. It was an experience I won't forget and it has helped me to understand the unique challenges on daily tasks that we may all take for granted.
Happy Lymphedema Awareness Month!!
Shoulder Rotator Cuff, Shoulder Impingement, and After Shoulder Surgery...
It is estimated that Rotator Cuff (RTC) Disease increases with age and affects roughly 4% to 32% of the population. The Rotator Cuff muscles and tendons keep your shoulder in its socket and much more. The Scapula also known as the "Shoulder Blade" is probably one of the most unassuming yet critical of all components of the shoulder. Most of the population believes it's just part of their back yet it is extremely complex. There are 18 Muscles that connect to the scapula but the specific muscles of "The Cuff" region: Supraspinatus, Infraspinatus, Teres Minor, and Subscapularis (SITS) join a set of critical tendons which are often what surgeons are assessing when they discuss Rotator Cuff (RTC) injury.
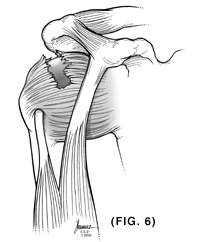
Shoulder Impingement is typically a compression or entrapment of the Rotator Cuff (RTC) Tendons leading to inflammation. This is happening roughly at the end of your collar bone by your shoulder joint. This is believed to be one way that the RTC Tendons become injured and even torn (other thoughts are aging, overload, etc..) Most often shoulder complaints from shoulder irritation are brought on through sports and occupation- the latter likely due to repetitive stresses. Raising the arms above shoulder level in an occupation or sport, regularly and repetitively, increases the probability of shoulder problems. Irrespective of initial insult to RTC tissues, poor movement patterns can exacerbate a shoulder problem and should be corrected. Sometimes we go from an inflamed tendon to a torn tendon because we don't address faulty movement patterns. *Cumulative trauma to RTC tendons are believed to cause the majority of Rotator Cuff Tears. (Fig.6)
The Rotator Cuff tendons are always at risk and should be protected through methodical shoulder movements, correct posture, stretching, and minimizing overuse and trauma. Forward slumped shoulders/posture closes the space around RTC tendons. Improper posture does play a role in shoulder pain and shoulder problems. Muscle weaknesses, muscle strength imbalances, poor posture/ form, injury, etc... all alter mechanical balances and load distributions which can negatively affect the Shoulder tissues leading to pain, weakness, loss of function, debilitation, and possibly surgery if not corrected.
Shoulder Physical Therapy Programs are often asserted to improve the area around the RTC Tendons and usually include highly specific stretching and strengthening. Initial goals may be to relieve pain but ultimately to correct dysfunction, return to proper functioning, and keep the RTC muscles and associated tendons safe from injury.
Post-Operative Shoulder Rehabilitation Programs are very specific to the surgeon and dependent on to what and where their repair is performed. Surgeons have their own protocol to follow after surgery and it is imperative to listen. Typically for a Rotator Cuff Repair the primary goal is maintaining the integrity of the repair while: gradually increasing Range of Motion, Lowering Pain and Inflammation, and minimizing Muscle Atrophy. Most RTC Rehabilitation protocols Do Not allow: heavy lifting, supporting bodyweight with hands and arms, jerking motions, nor excessive behind-the-back movements even at 6 weeks post-op. "Repair tissue does not reach maximal tensile strength for a minimum of 12–16 weeks post repair." (Int J Sports Phys Ther. 2012 April; 7(2): 197–218.) It is important to understand what "Passive Range of Motion" means. For a surgeon-defined time after your surgery, only your therapist will be moving your arm. This could be 4 weeks. In this defined time period the surgical repair site cannot stand active muscle contractions by the patient--the forces are too great on the surgical repair. Active motion of the arm by the patient is added later in your rehabilitation. Your Physical Therapist will carry out your surgeon's protocol so no worries.
Keep your shoulders healthy. One good practice is to "Love what You Lift" carrying objects close to your body. When surgery is needed listen to your Therapist and Surgeon carefully to guide you through Physical Therapy with the best results.
Rotator Cuff Tear. (Credit: Nature.com)
A little about that Trick Knee, OA, DJD, and ROM!
Knee Replacement , Knee Resurfacing, TKA, TKR, etc.... Approximately 650,000 of these were done in the year 2009. 63% percent of these were women and 96% were due to Osteoarthritis- aka, OA, DJD. DJD is "Degenerative Joint Disease" and this speaks to the nature of the condition. It is a normal aging process but you can definitely arm yourself to lessen the inflammation associated with this progressive condition.
Ok, so what do I do to take care of my knee and what should I expect if I do have surgery?
- irst, today you stand (or sit) with all of the physical experiences you have encountered dating back to your birth. This is deep, I know... Accumulative stresses and past injuries can result in dysfunction. If these affect the biomechanics of your knee it will likely lead to inflammation. So first thing is to make sure we are assessed by a Physical Therapist if your doctor suggests dysfunction. Recent research actually suggest Runners may not be accelerating Osteoarthritis as once believed. But there is research to support High Level athletes and Performing Artists accelerating Osteoarthritis., e.g, Soccer Players, Ballet Dancers, Weight Lifters, and Table Tennis players. It is likely that excessive "cutting", jumping, and rapid deceleration "degenerates" your joint while running has become a convenient scapegoat. See Links Page.
- o what is knee Range of Motion and why do I care? Well, you require a certain Arc at your knee to function- e.g., after Knee Replacement (TKA) many (but not all) people struggle for months to regain this Arc. One of the most important measures is getting it Straight! Why? Bend your knee for a prolonged period and feel your thigh wanting to burst. Straightening the knee moves a substantial load off the muscles. It has been my experience that most TKA surgeons expect the knee to be straight by one month post-op. All doctors have different protocols. Some use CPM machines and others do not. The most popular reason for a CPM seems to be early motion and blood clot prevention.
- What about bending my knee? If you notice, sitting in a chair requires the knee to bend 90 degrees. Climbing stairs requires about 80 degrees of bend. Furthermore, tying your shoe demands 117 degrees of bend at your knee. You can quickly see how important motion is to your everyday life. Knee Replacement Surgery restores substantial function and reduces pain according to The American Academy of Orthopedic Surgeons. Following surgery expect excessive Physical Therapy and the use of a cane or walker for weeks. Avoid Smoking as it slows healing. If you are not in Rehabilitation almost immediately after surgery-- ask questions... In the first month, typically there is no: jumping, kneeling, or bending.
- Can I prevent OA? Likely not as there is a genetic component and it is a natural aging process... But you could slow it down dramatically if you maintain proper form and function through your life while correcting your body mechanics as necessary through rehab--minimizing excessive "cutting" according to the research. Most knee replacements are metal. Through airports show your knee to inspectors. And a trick I noticed is that most airlines will allow the bag to be free of charge if you have a brace or medical device in your bag ;)
(Credit: American Association of Orthopedic Surgeons)
(Credit: American Association of Orthopedic Surgeons)
Lymphedema Awareness Month And Lymphedema D-Day
As of 2013, March is now known as Lymphedema Awareness Month. We are kicking off the month with a Blog post to raise awareness of the condition. On March 6th, The Lymphedema Awareness Community celebrates Lymphedema D-Day. This is the community's way of promoting awareness and change. This is also a way to promote better coverage for the condition through awareness and honor the patients who endure struggles with this condition. The National Lymphedema Network's (NLN) first D-Day was in 1994.
The NLN promotes Screening for Early Detection of Breast Cancer Related Lymphedema for better outcomes. In studies it has been shown that 32% of Breast Cancer Surgical Patients endure Persistent Swelling. A study in 2012 showed that Manual Lymph Drainage (MLD) essentially prevents this swelling when implemented after surgery. Wyatt Rehab Screens Breast Cancer Patients through Bioimpedance prior to surgery to establish a baseline so that post-operative swelling can be brought under control expeditiously through Manual Lymph Drainage as prescribed by your surgeon. Please read more about Wyatt's Breast Cancer Rehabilitation Program.
Joint Pain, Muscle Pain, Back Pain, Posture...
Whether discussing Acute Pain (rapid onset) or Chronic Pain (prolonged), we almost all experience it at some point. The problem with ignoring it is that often without intervention, the pain can cause loss of function, injury, and/ or disability. Perhaps the pain starts limiting your physical function and inhibits you from daily tasks like rising from a chair or even maneuvering stairs. The American Physical Therapy Association reports about 1/3 of all of us have back or joint pain. This is an alarming statistic.
This does not just happen in the elderly. This happens from the active to the inactive and we likely all know someone experiencing it right now. There is typically an underlying series of events that brought the pain on. This could be simply overuse or underuse. Often our bodies simply need to be re-educated. If we move early to correct this pain we can often avoid surgery and injury. If you look past symptoms, you can sometimes find faulty biomechanics that can be corrected with the proper Physical Therapy through a Rehabilitation Program.
Mechanical discrepancies within our bodies as the result of muscle imbalances can often be to blame for dysfunction. Think of your posture and how it affects your lower back and your neck. Sometimes muscles are shortened and tight while the opposing muscle becomes weak and elongated. This piggybacks off of the stretching blog I posted recently. Stretching in the proper manner can assist in rectifying these imbalances. I must emphasize proper manner as improper stretching can injure you. I recently heard a lecture that discussed a slumped inward posture even affects our hormones. This is likely why when people stand erect and talk on the phone they feel more confident than when they are sitting and slouched. Fatigue and depression seem associated with poor posture. Whether depression or hormones caused the poor posture is not the point. The point is that you are training your muscular and nervous system to follow this incorrect pattern that can lead to Pain.
Think about Golf or a Baseball pitcher. They are often using one side repeatedly and this can cause a one-side imbalance. For the most part our bodies crave symmetrical movements that allow normal function. Think of this next time you repeatedly do a movement within a single direction on a single side repetitively. Whether muscle lengths, scar tissue, or a host of other factors are causing you pain and dysfunction needs to be explored. Find out today and perhaps you can avoid future injury.
Wyatt Rehabilitation in West Long Branch, NJ now offers Yoga to improve Flexibility.
Stretching and Flexibility. Some general things to know…
Proper function of your muscles and joints demands enough range of motion in those joints--maintaining flexibility. Stretching that promotes persistent muscle length is essential!
Reduced flexibility is often seen over time and becomes much more apparent with the aged. When we couple this with reduced strength as we age, the result is decreased performance and an inability to perform daily tasks. Assessing flexibility is often difficult without a trained professional because many factors play a role including strength and disease (e.g. arthritis).
It is generally recommended that muscle temperature is raised through warm-ups prior to stretching. Stretch to your end range where tightness is felt. Do not induce substantial discomfort as you are more likely to injure yourself. Muscles are viscoelastic and inducing change in length comes with applied force but discomfort is your bodies way of saying, "slow down"... Changes in flexibility are not made overnight. Consistency and proper form are the most important aspects of stretching. Yoga is an excellent way to improve flexibility. Wyatt Rehab in West Long Branch, A Physical Therapy clinic known for its Breast Cancer Rehabilitation and Lymphedema Treatment, now offers Yoga to its patients partly because of the profound benefits in Range of Motion that can be achieved.
Stretching daily is recommended by most experts and each stretch should last approximately 15 seconds and need not exceed 30 seconds. Multiple stretches are recommended per muscle- a single stretch is beneficial but variety will incorporate more muscle groups. The stretching I am referring to is Static Stretching but other techniques exist as well. Dynamic and Contract/ Relax stretching exists but this is not recommended without professional input. The goal with stretching is consistency! This is so that improvements in both range of motion and function are maintained and not transient.
It is always recommended to consult your physician and physical therapist when engaging in these activities. This becomes essential when prior injuries or other conditions exist that could pose a risk to the individual.
A Day in the Life of a “Night Garment”
What is a “Night Garment”? When I first began treating Lymphedema, I never used the terminology “Night Garment”. I used to teach all patients how to remove the elastic compression garment that was worn during the day and then self bandage the limb at night before going to bed. Over the years, however, there has been a burst of alternative options to use in place of self-bandaging during Phase II of Complete Decongestive Therapy - Self-Care Management. I began referring to these garments as “Night Garments” because they are most commonly used at night during sleep.
Night garments can be described as alternative non-elastic compression garments that are made to replace bandaging in order to improve quality of life by making the process of compressing the limb at night easier and faster to apply. Over the years, I have been able to incorporate the use of so many of these night garments successfully in self-care management. I almost always recommend the option of using a night garment somewhere in the patient’s self care regimen because I feel it does allow the patient to be more compliant.
What I have learned by using night garments is that you must be attentive to how many hours you are averaging in the night garments per night. When I see patients for follow up in self-care management and they are struggling, I ask them a plethora of questions to figure out why their self-care regimen is not working for them.
Compliance to wearing the night garment every night is only one of the questions that should be asked during a self-care management follow up appointment with your lymphedema therapist. The most important question is how many hours are you averaging each night in the night garment? The reason why this question is so important is because some patients only sleep 3-4 hours a night. If a night garment is mistakenly understood as a garment to be worn only when you are sleeping, the affected limb may not be getting as many quality hours in the night garment as it should be.
This extremely important but simple question has solved issues that arise in self-care management much quicker. I make a conscious effort to educate my patients about how many hours of use are recommended for any of their compression garments when I am teaching them how to independently manage their swelling. I typically recommend that my patients shoot for 12 hours in the night garment which gives them less than 12 hours in the daytime elastic compression, given that you will be showering or cleansing the skin in between. This may vary per patient depending on the lifestyle, assistance needed, severity of lymphedema, and willingness to comply.
Some patients must use "night garments" 24 hours/day. Some other patients may only use the night garments when they need a break from self-bandaging for a night. Others may use the night garment during the day to add to the number of hours in a night garment within a 24-hour period. Regardless, it is important to ask your lymphedema therapist how long they recommend you use the night garment because success in self-care management could depend on it.
Because different patients perceived the use of the term “Night Garment” differently, I have changed my terminology with patients from “Night Garment” to “Alternative Compression Garment” or “Nonelastic Compression Garment”. This dispells any confusion or misunderstanding when instructing a patient when or how to use the garment.